In vivo models
Streptozotocin-Induced Diabetic Retinopathy
The Streptozotocin (STZ)-induced Diabetic Retinopathy model has been widely used in research for decades, with the first publications on STZ-induced diabetes appearing as early as the 1960s. This model is based on the ability of STZ to selectively destroy pancreatic β-cells, leading to chronic hyperglycemia and subsequent retinal complications. Over time, animals develop progressive retinal changes that mimic early-stage human diabetic retinopathy, including vascular leakage, pericyte loss, and inflammation. The severity of retinal pathology depends on various factors such as the STZ dose, animal species, and duration of diabetes. Due to its reproducibility and relevance to human disease, the STZ-induced diabetic retinopathy model remains a cornerstone for studying diabetes-related retinal dysfunction and evaluating potential therapeutic strategies.
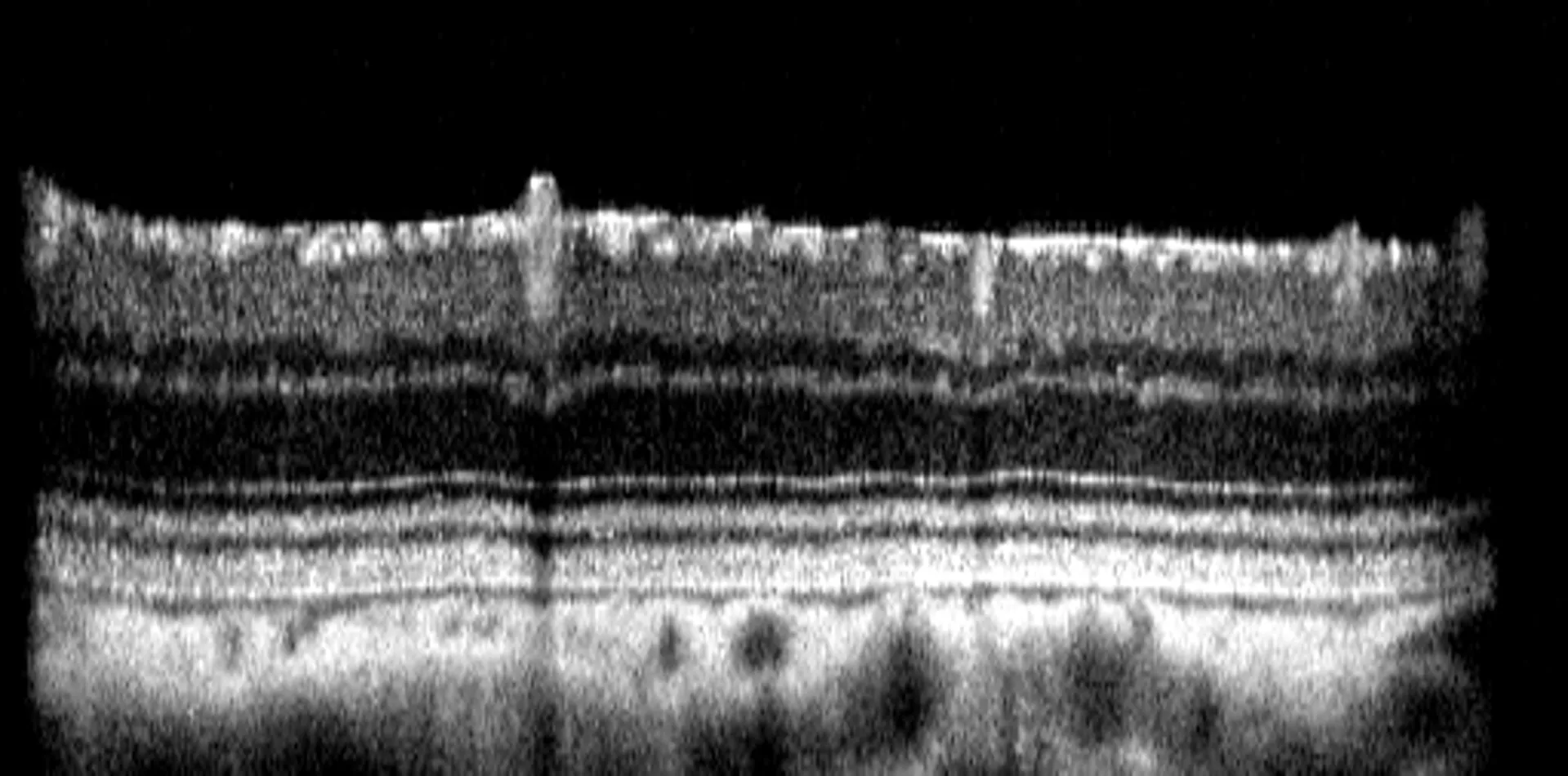
To track disease progression and evaluate treatment effects, Experimentica uses in vivo imaging and functional assessments for long-term monitoring of the STZ-induced diabetic retinopathy model. Spectral-domain optical coherence tomography (SD-OCT) captures high-resolution images of the retinal layers, allowing assessment of retinal thinning. Pattern electroretinography (pERG) evaluates retinal ganglion cell (RGC) function, while optomotor response test assesses visual acuity and contrast sensitivity.
Read more – discover our latest news on STZ-model!

Technical details
Mouse and rat
Intraperitoneal injection of STZ
Up to 16 weeks
Topical, intravitreal injection, intracameral injection, subretinal injection, systemic
– Glucose measurements
– Retinal layer thickness measurements (SD-OCT),
– Functional measurements (ERG, VEP),
– Behavioral assessment (visual acuity and contrast sensitivity)
– Immunohistochemistry
Highlights of this model
Clinically relevant
Mimics key features of human diabetic retinopathy
Reproducible & controlled
STZ reliably induces persistent hyperglycemia, allowing longitudinal monitoring and controlled disease progression.
Unbiased analysis
Quantitative readouts enabled by proprietary AI-driven algorithms.
References
- Pitale PM, Gorbatyuk MS. Diabetic Retinopathy: From Animal Models to Cellular Signaling. Int J Mol Sci. 2022 Jan 27;23(3):1487.
- Ragauskas S, Paulauskas T, Lelyte I, Neverauskas D, Mickevicius K, Cesna R, et al. Aflibercept exerts structural protection against diabetic retinopathy-associated inner retinal abnormalities in the mouse STZ model. Investigative Ophthalmol Vis Sci. 2023;64(556). ARVO Annual Meeting Abstract
Receive model details
Interested to learn more? Fill out the form below and we will email you a white paper on the disease model. Your information will not be added to any mailing lists or used for marketing purposes.
"*" indicates required fields
We are here to help
Whether you have a question about our preclinical models, capabilities, pricing or anything else, our team is ready to answer all your inquiries.
Related services
Flash Electroretinography
Flash ERG is a non-invasive method to assess retinal function in preclinical eye disease models.
Learn moreOptomotor Reflex
Experimentica offers behavioral assessment and optomotor response testing to evaluate visual acuity and contrast sensitivity in rodent models.
Learn moreIn vivo imaging
Experimentica offers extensive in vivo imaging capabilities for high-resolution ocular assessments across species.
Learn moreCheck out our latest news and activities
All News






